Clinical operations,
unified.
HIP One — Health Intelligence Platform unifies prior authorization, utilization management, medical review, payment integrity, and quality measurement on a single AI-native platform — powered by Aether One™ agents. Deployable across every shape (sovereign, government cloud, commercial cloud, on-prem). Consumable as a full platform or as individual agents.
PA productivity gain in clinical review
Satisfaction across active deployments
Auto-denials. Every non-affirmation routes to a human reviewer.
A healthcare brain
that turns prior auth into a defensible decision.
HIP One is one platform with three stages of clinical reasoning, wrapped around the Aether One™ core. Requests come in from any system. Decisions go out with a citation chain. Every non-affirmation is reviewed by a licensed clinician — by design.
Decisions in minutes, not days
Turnaround compressed from days of phone tag to a determination in minutes — without sacrificing rigor.
Every non-affirmation routed to a licensed clinician. By design.
No model unilaterally denies care. Mandatory human review on every potential adverse decision.
Audit-ready evidence trail for every decision
Each determination carries a cryptographic chain of citations — query-ready for appeals, regulators, internal audit.
Tuned per payer, plan, and line of business
Same engine, different policy packs. Stand up Medicare Advantage and Commercial in parallel without forking code.
Authorization request → defensible decision
Compliance is structural, not bolted on.
Every mandate that touches authorization — CMS, HIPAA, MHPAEA, MAC policy — wired into the engine, not patched on top.
Cross-cutting infrastructure for every module.
The same core that determines a $40k specialty Rx and a $4 generic — secure inference, versioned knowledge, defensible evidence.
A platform, not a point tool.
Healthcare organizations have lived with tight deadlines, manual processes, and scattered tools. HIP One replaces that stack. Each module is an Aether One™ agent surface — configurable, auditable, and shipped weekly.
Prior Authorization (PA)
Automatically route prior authorization requests from providers or members to the right department, the right reviewer, and the right outcome — with auto-affirm where evidence is unambiguous and human review on every clinical non-affirmation.
FHIR PAS · X12 278/275 · NCPDP SCRIPT
Medical Review & Clinical Decision Support
HIP One summarizes health records and acts as a clinical decision support system, surfacing case-specific insights from unstructured clinical documentation. Built on the same NLP that powers our PA decisioning.
C-CDA · CCD · PDF/Fax · DICOM metadata
Medicare STAR Ratings & HEDIS
Insights into Plan D and Plan C measures, plus the operational levers that move them. Outcome-aligned payment metrics for ACCESS Model participants are surfaced through the same module.
CMS-0057-F · ACCESS Model · OAT engine
Medical Record Digitization
Extract structured data from medical records, automate data entry, reduce errors, and improve compliance. The data layer that feeds every other HIP One module.
8 ontologies · 2.2M record vector store
Three integrated experiences. One end-to-end platform.
HIP One connects providers, service-operations teams, and clinical reviewers in a single end-to-end system. Each role gets the surface they need; every action lives in the same audit trail.
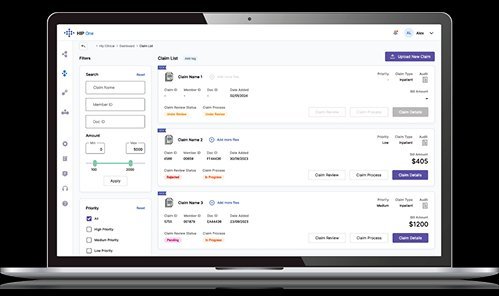
The provider-facing PA submission hub.
A secure, branded portal where providers submit standard prior authorizations, track real-time status, manage facility settings, and access decision letters — all in one place.
- Dashboard · drafts, in-review, recent decisions
- New PA submission · guided submission wizard
- Clinical details · diagnoses, codes, attachments
- PA status tracking · full lifecycle visibility
- Facility management · addresses, users, allowed domains
- Case management · ADR submissions, peer-to-peer
Other channels: fax, mail, direct integration.
PA intake, routing, and processing.
Service-operations teams receive, validate, and route inbound prior authorization requests to the right clinical queue — with real-time queue management and quality oversight.
- Intake dashboard · status, priority, workload
- Patient intake form · structured data capture
- PA routing & task flow · rule-based assignment
- Queue management · SLA-aware load balancing
- Quality & SLA metrics · live processing dashboards
- Throughput visibility · team and individual
Medical review and clinical decision.
Clinical reviewers assess submissions against medical-necessity criteria, issue formal decisions, and trigger compliant letter generation — with a full audit trail at every step.
- Medical review dashboard · SLA, priority, workload
- PA review — clinical details · full case context
- Clinical review workflow · structured decision flow
- Decision interface · affirmation, partial, non-affirm, dismissal
- Auto-triggered letters · provider and beneficiary
- Full audit trail · per-decision evidence chain
From provider submission to closed decision.
How a standard prior authorization moves through HIP One — one platform, one audit trail, five clear stages.
Submit PA
Provider submits via the portal — patient info, diagnoses, procedure codes, supporting clinical documents.
Intake & route
Service-operations team validates the submission and routes to the correct clinical reviewer based on PA type and payer.
Medical review
Clinical reviewer assesses medical necessity against criteria and issues a formal decision: affirmed, partial, non-affirmed, or dismissed.
Generate letters
Decision letters are automatically generated for the provider and beneficiary, and stored against the PA record.
Receive decision
Provider views the decision status and accesses letters directly on the portal dashboard. PA is closed.
Auto-deny is architecturally prohibited. Every clinical non-affirmation routes to a licensed clinician with a pre-built evidence package.
HIP One Summarization Agents turn dense CCDA records into clinical answers in seconds.
A generative-AI summarization agent inside HIP One. Extracts patient details, medication insights, and a navigable medical timeline from CCDA / C-CDA documents. Live on Microsoft Azure Marketplace and deployable standalone or as part of the platform.
- 01AI-Driven SummarizationConcise summaries from complex CCDA files
- 02Patient Data ExtractionDemographics, conditions, allergies, problem list
- 03Medication InsightsActive meds, dosing, prescriber, refills
- 04Medical TimelineChronological view of encounters and events
- 05Interactive ViewerSection-by-section navigation of source CCDA
Runs in customer's Azure environment. Full performance, scalability, and security.
Decision support, not decision-making.
Every clinical non-affirmation routes through Agent 871 (Non-Affirm Research) to a human reviewer. By architecture, not by policy.
| Capability | What it does |
|---|---|
| AI-powered decision support | For clinical nurses and medical directors. Surfaces evidence with provenance from the source document. Never surfaces a conclusion without showing its work. |
| Custom workflows | Tailored to payer or provider operating models — case routing, escalation paths, SLA tracking against CMS-mandated timeframes. |
| Seamless integrations | Epic, Cerner/Oracle Health, Meditech, Allscripts, eClinicalWorks, NextGen on the EHR side; Facets, QNXT, HealthRules, Amisys, Diamond on the payer side. |
| Clinical NLP | Extracts diagnoses, procedures, medications, lab values, and imaging findings from unstructured records. Trained on real clinical documentation, not generic web text. |
| FHIR-compliant APIs | CMS-0057-F day-one ready. CRD, DTR, and PAS in production. PA-RX adds NCPDP SCRIPT dual-channel for CMS-0062-P. |
| Scalable architecture | Adjusts to case volumes without resource strain. Sovereign-deployable for government health programs. |
What buyers ask first.
Who is HIP One for?
Health plans, health systems, MACs, and other healthcare organizations that need to unify clinical, operational, and financial workflows. It replaces fragmented PA + UM + medical-review point tools with one integrated system.
What's the regulatory posture?
CMS-0057-F compliant in production. CMS-0062-P channel architecture filed in PA-RX. WISeR Model deployment partner. HIPAA Security Rule 2026 updates supported via CPS One co-deployment.
What results have early users seen?
42% productivity gain in clinical review. Faster turnaround. Measurable reduction in delegated UM dependency. Government deployment running on sovereign infrastructure.
Can we deploy in our own environment?
Yes — sovereign/on-premise, private cloud (AWS, Azure, GCP), or multi-tenant SaaS. CMS WISeR runs HIP One on government-compliant infrastructure today; the same code path supports payer environments.
Four steps to live deployment.
A predictable engagement path. No "scope a six-month POC" runway. From first conversation to production, with clear gates at each step.
Schedule a live demo
Walk through the platform with the team that built it. 45-minute working session against your real use case.
Review integration requirements
Map the platform to your existing systems — EHR, payer admin, telephony, identity, data warehouse. Document gaps.
Pilot with your data
Stand up a scoped pilot in your environment. Real data, narrow surface area, measurable outcomes from day one.
Deploy & go live
Production rollout with full audit posture, rule-pack governance, and the support model your team needs.
Key team members.
Architecture and delivery leadership for the Health Intelligence Platform — from agent design through live customer deployment.


Walk through HIP One with the team that built it.
45 minutes. Live, NCD-traceable rule packs running against published clinical guidelines. Your specific use case — whether that's payer UM consolidation, provider PA submission, or government Medicare program participation.